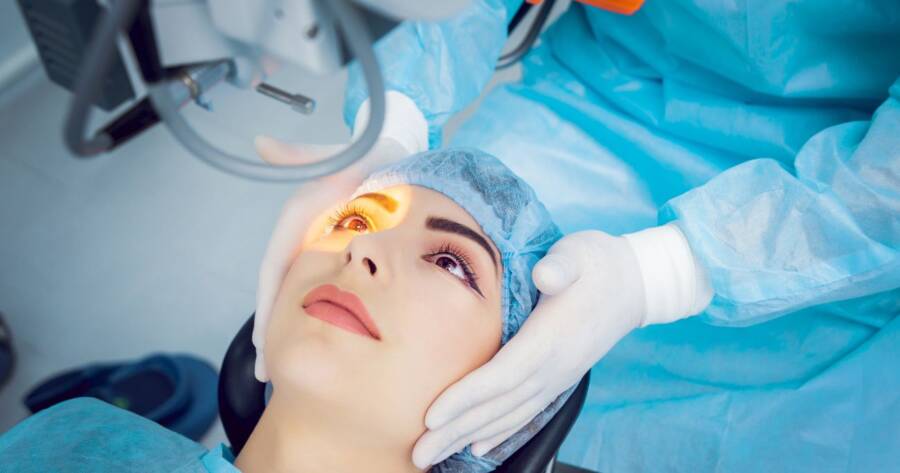
- Cataracts commonly affect adults later in life but are easily removed with cataract surgery if they interfere with daily tasks and activities.
- Cataract surgery involves creating an incision with surgical or laser tools, removing the cataract and replacing it with an artificial lens.
- The cost of cataract surgery depends on factors such as the surgical technique, type of artificial lens and the surgeon you choose, but it may be covered by your insurance plan.
Cataracts are a common issue later in life and one of the world’s leading causes of blindness. Although you may not notice a cataract right away, they can make everyday activities more challenging and sometimes hazardous.
Cataract surgery can correct vision problems related to cataracts. Here’s what you should know about cataracts as well as the process and costs for cataract surgery.
What Is a Cataract?
A healthy lens in your eye is clear, but as you age, the proteins in your eyes may break down and clump together to create a cloudy or blurry area called a cataract. In addition to general vision loss, you may notice color dullness, reduced contrast sensitivity and loss of color perception. This can mean you’re unable to see well at night, lights appear too bright, and you may even have double vision.
Certain factors can put you at higher risk for developing cataracts, including:
- Smoking;
- Excessive alcohol consumption;
- UV ray exposure;
- Family history of cataracts;
- Diabetes;
- Radiation treatment for cancer, and;
- Eye injuries.
What Is Cataract Surgery?
Certain treatments, such as lifestyle changes or new prescriptions, can help manage cataracts, but cataract surgery is the only way to get rid of them. During cataract surgery, your surgeon removes the cloudy lens from your eyes and replaces it with an artificial lens, also called an intraocular lens (IOLs).
Most patients are conscious throughout the procedure but can’t see what the surgeon is doing. During the procedure, your surgeon first applies drops in your eyes to dilate and numb your eyes, and they may offer a sedative to help you relax. They then use small tools to remove the cloudy lens and replace it with an artificial lens. Cataract surgery typically only takes about 30 minutes.
Types of Cataract Surgery
The most common type of cataract surgery is phacoemulsification, which uses ultrasound energy to emulsify the eye’s lens. The surgeon first makes one or more incisions in the eye using surgical tools or lasers and then removes the anterior part of the capsule that contains the lens. To emulsify the lens, the surgeon uses an ultrasonic handpiece with a titanium or steel needle that vibrates and pumps aspirated particles through the tip. Once the cataract is broken down, each piece can be aspirated with suction.
Extracapsular cataract surgery is generally reserved for advanced cataract cases that are too dense for phacoemulsification treatment. Surgeons create a larger incision to remove the cataract in one piece, insert an artificial lens and close the wound with sutures.
Types of IOLs
There are several types of IOLs to choose from when removing a cataract, and each comes with specific benefits. The main types of IOLS are:
- Monofocal: Can be used to treat nearsightedness, farsightedness or contrast issues but can’t resolve astigmatism. They are covered by many insurance plans, but you may need glasses for other vision issues.
- Multifocal: Provide greater potential to see at more than one distance, reducing the need for glasses or contacts. They may not be suitable for patients with significant astigmatism or eye trauma.
- Toric: Can reduce or eliminate astigmatism as well as the need for glasses or contacts.
When You Need Cataract Surgery
Cataracts don’t always require surgery and can be managed with lifestyle adjustments, prescription eyewear or better lighting. If your symptoms increase and interfere with activities or even make tasks such as driving or work dangerous, it might be time for surgery.
Your doctor may also recommend cataract surgery even before it interferes with your lifestyle. Cataracts can grow large enough to crowd the inside of the eye and increase uncomfortable pressure. It may also be necessary to have cataract surgery if a cataract is interfering with the treatment of other eye problems or making eye examinations difficult to perform.
Cataract Surgery Risks
Lasting or serious side effects and complications after cataract surgery are rare. Cataract surgery risks include:
- Swelling;
- Inflammation;
- Bleeding;
- Infection;
- Dislocation of artificial lens;
- Retinal detachment;
- Drooping eyelid;
- Glaucoma;
- Secondary cataract;
- Vision loss, and;
- Light sensitivity.
Certain factors may increase the risk of complications, including other eye problems or serious medical conditions. It’s also possible to have allergic reactions to anesthesia. Some itchiness, watering or discomfort is normal after surgery, but you should contact your doctor if symptoms persist or worsen.
Choosing a Surgeon
If your current eye doctor is an ophthalmologist, they may be able to perform your cataract surgery. If they’re unqualified or you don’t feel comfortable having them perform your surgery, you’ll need to find a trustworthy cataract surgeon.
Cataract surgeries are low-risk procedures, but an unsuccessful surgery can have lasting consequences. Get ophthalmologist referrals from your doctor, friends and family, check for surgeon testimonials and reviews and ask them as many questions as needed to feel comfortable and safe in the procedure. Consider questions such as:
- How many cataract surgeries have you performed?
- What kind of vision results do they expect from the procedure?
- What type of IOLs do they recommend?
- What does surgery aftercare look like?
- How many of their patients experience complications?
Pre-Surgery Tests
About a week before the surgery, your doctor measures the size and shape of your eye with a noninvasive ultrasound test to determine the right type of artificial lens.
Some surgeons use laser technology to measure the length of the eye, which can be even more accurate than ultrasound tests. Although it may cost more, this option can reduce the need for glasses after surgery.
Doctors can also use wavefront analysis to measure unique variations and irregularities in the cornea, resulting in a detailed and precise assessment of the eye. This test involves resting your chin on a device and staring past a target light as a sensor measures light reflecting from your cornea.
Tests such as EKGs, blood tests and x-rays are typically unnecessary.
Before Surgery
In addition to testing, your surgeon will ask about any medications you’re currently taking, as they may interact or interfere with your surgery or recovery. For instance, doctors typically recommend discontinuing blood thinning agents at least a week before surgery.
To prevent swelling, infections or other post-surgery issues, your surgeon may prescribe antibiotics or steroid eye drops to use for a day or two before and after the procedure. They may also instruct you to not drink or eat anything 12 hours before the surgery.
Surgery Recovery
Immediately after the surgery, your vision may seem distorted, and you’ll likely experience mild discomfort as your eye adjusts to the new IOL. You may have bloodshot eyes or bruising from the anesthesia injections.
Although many patients report clear vision within a few hours after surgery, you won’t be able to drive for several days. You should avoid heavy lifting, pressure on your eyes and any other strenuous movement. Your surgeon may provide you with a protective eye cover to wear at night for a few weeks.
It can take up to eight weeks to fully recover from surgery. If you received stitches for your procedures, your surgeon would remove them a few weeks after surgery.
Cataract Surgery Results
Cataract surgery restores vision in most people who undergo the procedure, but you may still need to wear glasses or contact lenses depending on the IOLs and surgical technique. Your doctor can assess your healed vision between one and three months after surgery to determine an eyeglasses prescription.
In some cases, a cloudy layer or secondary cataract may appear after surgery. This is called posterior capsule opacification (PCO) and occurs when the back of the lens capsule becomes cloudy. Your doctor can easily treat PCO with a brief and painless treatment called yttrium-aluminum-garnet (YAG) laser capsulotomy, which uses a laser to make a small opening in the capsule and a clear path for light to pass through.
Surgery Costs
Costs for cataract surgery can depend on several factors, including the type of IOL, surgical technology used and the surgeon you choose. Private medical insurance often covers standard cataract surgeries with monofocal IOLs, so it’s possible to have no expenses for the procedure other than your deductible or copayments. Aside from the procedure and IOL, you may also need to pay for pre-surgery tests, eyeglasses, contact lenses and other costs.
If you don’t have insurance or opt for more expensive procedures, such as laser cataract surgery and more expensive IOLs, you may need to pay for the associated costs. Around the world, the mean costs of cataract surgery range from $2,608.81 to $7,838.61. In the United States, the average out-of-pocket cost per eye is $3,500 as of 2021.