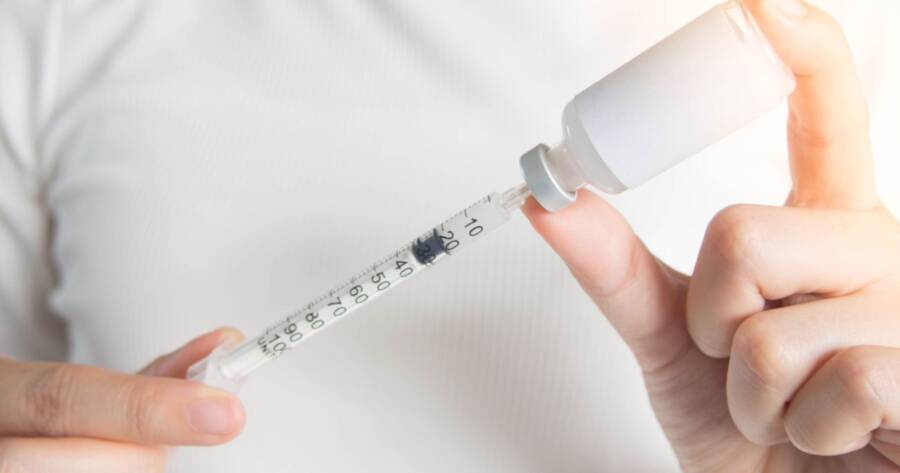
When it comes to insulin, though, even innocent oversights can be dangerous or fatal. Keep reading to learn about the most common mistakes you can make with insulin and how to avoid them.
When your body doesn’t produce enough insulin or fails to properly utilize it, synthetic insulin is a lifesaver. Every day, around six million Americans depend on it to keep blood sugar levels in check. Life is just as busy for them as it is for everyone else. Even well-intentioned patients forget doctor appointments, postpone exercise, and lose track of time.
Adjusting Your Own Dose
It’s a mistake to adjust your insulin dose when you indulge in sweets. At best, you’ll require larger doses over time. At worst, toying with the prescribed dose can endanger your health. No one disputes the fact that it takes discipline to eat well and stay away from foods that your doctor has prohibited, but it’s well worth the effort.
It may seem logical to skip or reduce doses when you’re sick, but that’s also a bad idea. You still need insulin when you’re vomiting or have diarrhea; blood sugar levels can spike if your body is under stress.
Talk to your doctor ahead of time about how much insulin to use when you’re sick and have little food in your digestive tract. Schedule an urgent appointment if you have any of the following symptoms:
- Vomiting or diarrhea lasting more than six hours
- A blood sugar level above 240 even when you’ve taken the recommended sick-day dose
- Symptoms of dehydration or ketoacidosis, which include dry mouth or lips, difficulty breathing, fruity-smelling breath or chest pains
Innocent dosage mistakes happen too. There are four distinct types of insulin. It’s easy to get confused and take the wrong type, especially if your doctor has prescribed more than one. Keep different insulins separate, perhaps using a color-coded labeling system, and pay good attention at injection time.
Not Carrying Medication
Even when you dash out of the house on a quick errand, carry your next insulin dose. You never know when you’ll get stuck in traffic or a long line at the grocery store.
It goes without saying that you should always wear an identifying diabetes tag. In the event of an emergency that renders you unconscious, medical personnel will know at a glance how to provide the best care.
Losing Track of Your Schedule
It’s easy to become preoccupied with carpool duties, vet appointments, yard work, and other day-to-day business. Soon enough, you snap to and struggle to remember whether you took your last dose of insulin.
Set an alarm clock or program automatic alerts on your smartphone. Record doses and times taken in a purse or pocket notebook. Be sure that you fully understand how long various types of insulin stay in your system so that you’ll know when it’s safe to take more.
Storing Incorrectly
The importance of correctly storing insulin can’t be overstated. Its potency declines when it’s exposed to extreme temperatures. The longer it stays too hot or too cold, the less effective it is. The ideal place for unopened insulin is in the refrigerator. Maintain a consistent temperature somewhere between 36 F and 46 F. Store opened vials in the fridge or at a cool room temperature. They will stay potent for up to 28 days.
Don’t expose insulin to direct sunlight. If you’re traveling with it, don’t store it in a hot glove compartment or allow it to freeze in a cooler.
Never use insulin that has expired, been allowed to freeze or been stored at room temperature longer than 28 days. Before each use, check the vial for discoloration, frost, clumps, or foreign particles. Throw it out if necessary.
It’s best to purchase a monthly supply of insulin rather than stockpile it. Expired product must be discarded.
Exercising Carelessly
Consistent, carefully planned exercise is one of the best tools for managing diabetes. Physical activity helps your body use insulin properly and decreases resistance to it. Failing to take exercise seriously almost always leads to complications.
Even brisk walks lasting 10 to 15 minutes help control blood sugar. Not only that, but frequent, regular exercise wards off obesity, heart disease, stroke, depression, insomnia, and other major barriers to health and well-being.
Shoot for around 150 minutes a week. People who schedule exercise and work out at the same time every day are more likely to maintain good health. Here are some ideas for achieving your fitness goals:
- Fast-paced walking
- Light jogging
- Bike riding
- Rowing
- Tennis
- Swimming
- Water aerobics
There are a few precautions you should take.
Don’t allow your blood sugar level to drop too low while you’re exercising. If it’s below 100, eat about 30 grams of carbs before you start exercising.
Check your blood sugar level every hour during exercise. Always keep a carbohydrate snack with you in case it drops too low during your workout.
Check levels again when you finish your workout and periodically for the next few hours. It’s possible to have a delayed drop after exercise.
Taking your injection in a spot that’s used heavily during exercise can result in the insulin being absorbed too quickly. For instance, don’t inject your thigh if you’ll be running or cycling.
Track your body’s reactions to exercise and discuss them with your doctor. If blood sugar levels frequently run high or low after physical activity, the doctor can pinpoint exercise behaviors that are upsetting the balance or adjust your insulin dose.
Eating Irresponsibly
Never use foods that you crave to correct a sudden drop in blood sugar. You may not be able to put down that pint of ice cream. Then, your insulin won’t be able to do its job, and you’ll be worse off than before.
It’s best to get rid of the ice cream altogether. If you can’t part with it, at least reach for doctor-approved snacks when you need to boost your blood sugar. Even healthy snacks are prone to abuse. Control your portions by using single-serving-size food storage bags.
Avoid dangerous blood sugar spikes by checking levels 15 to 30 minutes before meals. Inject a bolus if necessary.
Skipping Doctor’s Appointments
Professional monitoring of your condition is crucial. Failing to keep your routinely scheduled appointments can lead to severe or life-threatening complications.
Appointments with other specialists, such as your dentist and podiatrist, are almost as important. The various systems in your body are designed to function together for overall good health. When one is neglected, others will quickly decline. It’s a domino effect.
Another advantage to a well-rounded approach is that it keeps all your caregivers on the same page to provide you with the best treatment. If one doctor tries a new medicine or therapy, be sure to communicate it to all the others.
Hardly anyone says that diabetes is a breeze to manage, but avoiding common mistakes makes life much easier. If you do flub up, call your doctor and confess right away.
 Orawan Pattarawimonchai / Shutterstock
Orawan Pattarawimonchai / Shutterstock